


Driving Precision in Robotic Surgery:
The Impact of Catheter Materials

Robotic surgical systems are built to deliver stability, precision, and safer interventions across a growing range of clinical applications—from neurovascular and pulmonary procedures to cardiac and electrophysiology interventions. While the robotic platforms themselves continue to advance, much of their real-world performance depends on the devices that enter the body. Catheters, in particular, play a critical role in translating robotic motion into controlled, reliable clinical action, delivering precise force transmission, targeting, and responsiveness as they navigate complex anatomy.
As robotic surgery evolves, catheter design has become more complex. These devices must navigate tortuous anatomy, integrate electronics and sensors, tolerate repeated sterilization, or enable single-use workflows, and maintain mechanical performance across demanding environments. Meeting those requirements is more than a design challenge—it is a materials and manufacturing challenge that directly affects how quickly new robotic technologies can reach scale.
Robotic-assisted procedures place unique demands on catheter systems. Unlike traditional manual devices, robotic catheters must deliver consistent, predictable, and repeatable performance under precise mechanical control. Pushability, torque response, and distal flexibility all need to be carefully balanced to help enable accurate navigation without compromising patient safety.
Many of these requirements mirror those found in minimally invasive catheter applications, but robotic systems often demand higher levels of precision and control. Catheters may need to support articulation, steerability, and fine positional control while integrating additional functionality such as sensors, fiber optics, cameras, or electrodes. As robotic platforms expand into more procedures, the catheter becomes a multifunctional system rather than a passive conduit.
While biocompatibility remains a fundamental requirement, ensuring durability, reliability, and consistent performance becomes equally important—especially as devices are exposed to repeated sterilization cycles, harsh cleaning chemistries, or complex clinical workflows. These factors place significant pressure on material selection and construction methods.
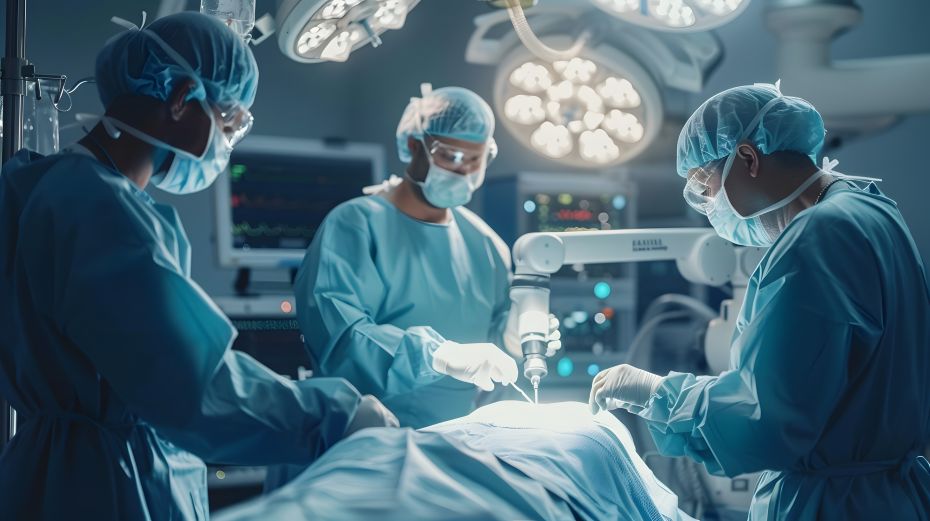
Material choice directly shapes how robotic catheters perform in clinical use. Polymers used in these applications must balance flexibility and strength while maintaining their properties over time. Sterilization alone introduces a wide range of stresses. Multiple cycles of heat, chemicals, and moisture can alter mechanical properties, particularly in softer materials used at the distal end of the catheter.
Key material considerations include:
For these reasons, higher-performance polymers such as fluoropolymers (including PTFE and FEP), PPSU, and PEEK are commonly used in robotic surgical components. PEEK, in particular, has become a go-to material for applications requiring high strength, chemical resistance, and thermal stability. In some cases, glass-filled PEEK grades are used as lightweight metal replacements, providing durability across repeated use and sterilization cycles.
At the distal end of the catheter, however, ultra-soft materials remain essential. These materials enable atraumatic navigation but are more susceptible to degradation. As a result, many designs are moving toward hybrid approaches, combining reusable proximal components with disposable distal sections to balance performance, safety, and lifecycle considerations.
As robotic surgery increasingly incorporates electrophysiology, sensing, and energy delivery, dielectric performance has become a critical design consideration. Catheters must insulate sensitive electronics and prevent interference with other devices in the operating room.
Polyimide has emerged as a gold standard material in this area due to its exceptional dielectric strength and ability to be manufactured with extremely thin walls. Typically, produced through a layered dipping process rather than extrusion, polyimide enables low-profile designs while maintaining flexibility and electrical insulation. These properties make it well suited for catheters that integrate sensors, electrodes, or fiber optics.
Composite material approaches are also gaining traction. By reinforcing polymers with glass fibers or combining materials with complementary properties, manufacturers can achieve higher tensile strength, improved durability, and tailored mechanical performance. These advances allow designers to fine-tune catheter behavior along its length—stiffer proximally, softer distally—while supporting increasingly complex robotic functions.
Sterilization challenges, infection risk, and hospital workflow pressures are driving a broader shift toward more efficient single-use devices in certain robotic applications. Reprocessing complex devices with small lumens and articulated sections is labor-intensive and difficult to validate, increasing the risk of biofilm formation and hospital-acquired infections.
Fully disposable systems can reduce these risks but introduce new challenges related to cost, waste, and sustainability. Medical devices cannot easily incorporate recycled materials due to biocompatibility concerns, making material efficiency and thoughtful design even more important.
Hybrid approaches—where reusable components are paired with disposable distal elements—often offer a practical compromise. For example, in neurovascular catheters, the ultra-soft distal tips must navigate delicate vessels and are highly sensitive to repeated sterilization, making them ideal candidates for disposability. Similarly, in electrophysiology catheters, distal segments integrating sensors or fiber optics can be designed as single-use components, while the proximal handle or robotic interface remains reusable. These designs allow manufacturers to leverage durable, high-performance materials where reuse is practical, while minimizing infection risk and performance degradation in the most sensitive parts of the device.
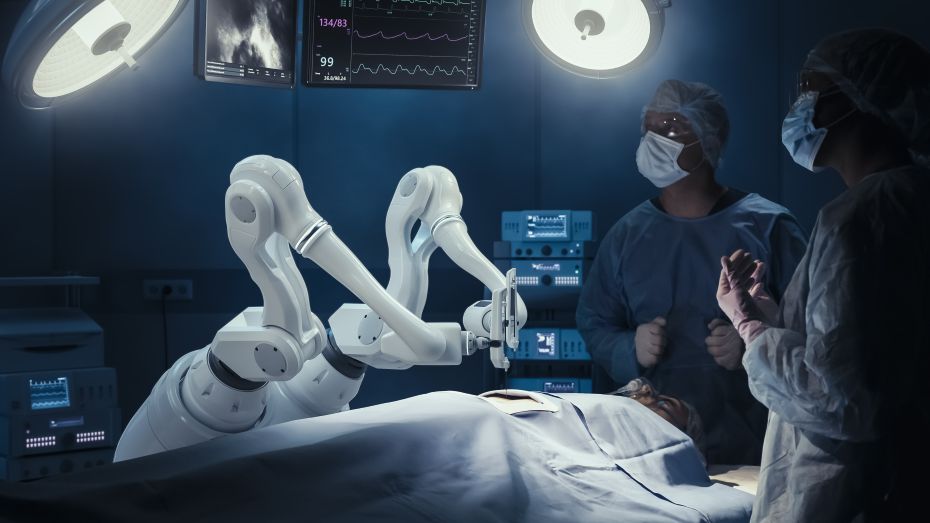
Bringing robotic catheter technologies to market often involves significant pressure to accelerate development, but early decisions—while necessary for progress—can have significant consequences, especially when scaling to higher volumes. Many challenges that emerge post-launch—such as yield loss, variability, or capacity constraints—can be traced back to development choices driven by time and cost pressure.
Material variability is a common issue, particularly with polymers. Validating a process across only part of a material’s allowable range can lead to performance problems once production expands. Understanding melt flow variability, long-term material behavior, and supplier consistency is critical when designing scalable processes.
Equipment and process repeatability also matter. A manufacturing process that works for short development runs may not hold up under extended production cycles. Extrusion lines, bonding equipment, and lamination processes must be capable of running longer hours without degradation or frequent downtime.
People and training are another critical factor. Many catheter manufacturing steps remain highly specialized and operator-dependent. Fatigue, ergonomics, and skill availability can all impact quality and throughput. Identifying which processes are most sensitive—and where automation or semi-automation can be strategically implemented—can significantly improve scalability and consistency.
Finally, establishing precise acceptance criteria early in development—beyond basic dimensional tolerances—helps allow smoother transitions from development to production. As much as possible, limited sample images should be retained during process development and used to define acceptability for any subjective quality inspections.
In robotic surgery, innovation depends on the seamless integration of materials science, technical expertise, design, and manufacturing. Catheters sit at the intersection of these disciplines, presenting significant engineering challenges while enabling precise device performance. Their design and construction directly influence flexibility, strength, durability, and responsiveness—factors that ultimately determine how safely and effectively a surgeon can navigate complex anatomy.
OEMs that engage manufacturing partners early—aligning on material selection, validation strategies, and scalability requirements—are better positioned to move quickly without sacrificing reliability. By designing catheter systems that account for real-world use, sterilization, and production demands, teams can reduce downstream risk and accelerate adoption.
As robotic surgery continues to expand, the role of catheter materials and manufacturing strategies will only grow in importance. Precision in the operating room begins long before a procedure starts—it begins with the decisions made at the material and process level that ultimately determine how fast innovation can move, and how reliably it can scale.
David Kramer - Engineering Director, Healthcare Solutions, DuPont
Joseph Bogusky - Staff Mechanical Engineer, Intuitive Surgical
Steve Maxson - VP of Growth, Chamfr